Wednesday, September 19, 2012
Folliculitis
Folliculitis
Localized inflammation of a hair follicle. The condition may be caused by infections, injury or irritation and is generally found on the face, neck, breast and buttocks. The damaged follicles are then infected with the bacteria Staphylococcus (staph).
The condition may be caused by staph aureus, yeast or fungi. If the condition spreads or becomes persistent swab cultures may need to be taken.
Lymphedema patients are more susceptible to skin infections and are strongly advised against hot tubs because of the possibility of contracting Pseudomona folliculitis. This is a resistant gram-negative bacterial infection with serious complications. Barber's itch is a staph infection of the hair follicles in the beard area of the face, usually the upper lip. Shaving makes it worse. Tinea barbae is similar to barber's itch, but the infection is caused by a fungus.
Pseudofolliculitis barbae is a disorder that occurs mainly in black men. If curly beard hairs are cut too short, they may curve back into the skin and cause inflammation.
Clinical:
Pus in the hair follicle
Irritated and red follicles
Damaged hair (possibly in growing back into the follicle)
Complications:
While we tend to think of folliculitis as a minor and superficial infection, it is important to remember that with a lymphedema limb that is immunocompromised, the folliculitis could develop into a more severe infection. Complications include cellulitis, forunculosis (This condition occurs when a number of boils develop under your skin. Boils usually start as small red bumps but become larger and more painful as they fill with pus), scarring, destruction of the hair follicle. Untreated and/or severe/deep folliculitis could result in sepsis and bacteremia.
Treatment:
Topical antibiotics which may include bacitracin, polymyxin B sulfate (Polysporin), clindamycin, erythromycin, or mupirocin (Bactroban). You may also use an antiseptic cleanser, such as povidone-iodine (for example, Betadine) or chlorhexidine.
Oral antibiotics based on the seriousness (deeper or more severe infections) of the folliculitis or on the underlying medical condition of the patient. If caused by a bacteria, your doctor may prescribe dicloxacillin, erythromycin, or cephalexin (such as Keflex). Ciprofloxacin (Cipro) and ofloxacin (such as Floxin) are used for certain types of bacteria.
Fungus based folliculitis is treated with antifungal oral medications which include You will need to take antifungal pills, such as fluconazole (Diflucan), griseofulvin (Fulvicin-U/F or Gris-PEG, for example), itraconazole (Sporanox), or terbinafine (Lamisil).
Full Text Page
Erysipelas
Erysipelas
Key Words: Strep A, Lymphedema, Cellulitis, Bacteremia, Septicemia, Cutaneous lympatics, immunocompromised, St. Anthony's Fire, Staph aureus, Strep G, Penicillin, Probenecid, Dicloxacillin, Erythromycin, Keflex, Augmentin, Necrosis, Gangrene, Thrombophebitis, Bacterial endocarditis, Soft tissue infections
Discussion
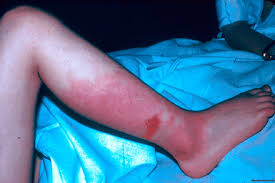
Erysipelas (also called St. Anthony's Fire)is a superficial bacterial skin infection skin generally caused by (Strep A bacteria or Strep B bacteria. It can spread with alarming rapidity as it invades the cutaneous lymphatics.
While some classify it as a "form of cellulitis," it actually can be differentiated by the clear lines of demarcation of the infection. Symptoms include marked lines of infection, fever, pain, an overall achy feeling and swollen lymph nodes. Most cases involve the legs, and the second largest number of cases involve the face. However a delay in treatment can result in deeper cellulitis or lymphangitis.
Like any type of infection a lymphedema patient experiences, antibiotic treatment needs to start immediately so as to prevent septicemia or bacteremia. As with any infection erysipelas present a serious threat due to the immunocompromised state of the lymphedemous limb and because possible fibrosis handicaps effective antibiotic therapy. Also, in lymphedema patients Staph aureus (not Strep A) has been implicated as the infective bacteria.
While very similar and often confused with actual cellulitis it can be differentiated by the raised borders and advancing edges. The most commonly affected body areas are the legs, followed by the face.
Risk Factors
There are a number of factors that might predispose one to erysipelas. The primary cause of course is a break, cut or entry foci in the skin and subsequent infection usually by a Strep A bacterium. Susceptibility factors include edema, lymphedema, venous insufficiency, venous stasis, dermatosis, diabetes, HIV infection, and other immunocompromising medical conditions.
Transmission factors include port of entry through nasal cavity, insect bites, cut, incisions.
Symptoms
The infection may start out as a inconspicuous small red patch and spread rapidly to a painful fiery red plaque. The infection area will be warm or hot and quite tender. Over-all body symptoms might include feeling unusually drained of energy, achiness, chills, fever and malaise. There may also be blisters on the infected area and possible red streaking.
Treatment
Treatment generally will involve the administration of an oral antibiotic. The infection responds well to penicillin based antibiotic. In addition Probenecid may be used as it increase the effectiveness of penicillins. For more resistant infections dicloxacillin may be used. Other antibiotics may include Nafcillin, Erythromycin, Keflex and Augmentin.
Depending upon the severity and spread IV antibiotic therapy may also be used for lymphedema patients. Also, limiting one's activity with limb elevation is standard protcol.
Blood cultures and/or wound cultures may be needed to determine the exact bacteria involved.
Complications
Complications may include bacteremia or septicemia, abscess, tissue necrosis (gangrene)in the most severe cases, thrombophlebitis, bacterial endorcarditis.
Prognosis
Prompt diagnosis and treatment will bring favorable results and in all but a very few patients recovery will be complete and without complications. At risk groups, including those with lymphedema may experience recurrent episodes.
Full Text

Key Words: Strep A, Lymphedema, Cellulitis, Bacteremia, Septicemia, Cutaneous lympatics, immunocompromised, St. Anthony's Fire, Staph aureus, Strep G, Penicillin, Probenecid, Dicloxacillin, Erythromycin, Keflex, Augmentin, Necrosis, Gangrene, Thrombophebitis, Bacterial endocarditis, Soft tissue infections
Discussion
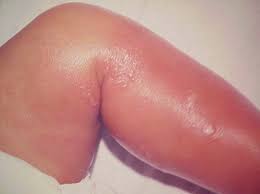
Erysipelas (also called St. Anthony's Fire)is a superficial bacterial skin infection skin generally caused by (Strep A bacteria or Strep B bacteria. It can spread with alarming rapidity as it invades the cutaneous lymphatics.
While some classify it as a "form of cellulitis," it actually can be differentiated by the clear lines of demarcation of the infection. Symptoms include marked lines of infection, fever, pain, an overall achy feeling and swollen lymph nodes. Most cases involve the legs, and the second largest number of cases involve the face. However a delay in treatment can result in deeper cellulitis or lymphangitis.
Like any type of infection a lymphedema patient experiences, antibiotic treatment needs to start immediately so as to prevent septicemia or bacteremia. As with any infection erysipelas present a serious threat due to the immunocompromised state of the lymphedemous limb and because possible fibrosis handicaps effective antibiotic therapy. Also, in lymphedema patients Staph aureus (not Strep A) has been implicated as the infective bacteria.
While very similar and often confused with actual cellulitis it can be differentiated by the raised borders and advancing edges. The most commonly affected body areas are the legs, followed by the face.
Risk Factors
There are a number of factors that might predispose one to erysipelas. The primary cause of course is a break, cut or entry foci in the skin and subsequent infection usually by a Strep A bacterium. Susceptibility factors include edema, lymphedema, venous insufficiency, venous stasis, dermatosis, diabetes, HIV infection, and other immunocompromising medical conditions.
Transmission factors include port of entry through nasal cavity, insect bites, cut, incisions.
Symptoms
The infection may start out as a inconspicuous small red patch and spread rapidly to a painful fiery red plaque. The infection area will be warm or hot and quite tender. Over-all body symptoms might include feeling unusually drained of energy, achiness, chills, fever and malaise. There may also be blisters on the infected area and possible red streaking.
Treatment
Treatment generally will involve the administration of an oral antibiotic. The infection responds well to penicillin based antibiotic. In addition Probenecid may be used as it increase the effectiveness of penicillins. For more resistant infections dicloxacillin may be used. Other antibiotics may include Nafcillin, Erythromycin, Keflex and Augmentin.
Depending upon the severity and spread IV antibiotic therapy may also be used for lymphedema patients. Also, limiting one's activity with limb elevation is standard protcol.
Blood cultures and/or wound cultures may be needed to determine the exact bacteria involved.
Complications
Complications may include bacteremia or septicemia, abscess, tissue necrosis (gangrene)in the most severe cases, thrombophlebitis, bacterial endorcarditis.
Prognosis
Prompt diagnosis and treatment will bring favorable results and in all but a very few patients recovery will be complete and without complications. At risk groups, including those with lymphedema may experience recurrent episodes.
Full Text
Subscribe to:
Posts (Atom)
